Competing with Pulmonarymucormycosis for rescuing time
Nov 17, 2023 Zybio News
-

December 26, 2025
DiagHub Online Academic Platform The ninth session on Microbiology Concludes Successfully – Highlights Recap
-

Nov 28, 2025
DiagHub Online Academic Platform The eighth session on Molecular Concludes Successfully – Highlights Recap
-

Nov 21, 2025
Zybio at MEDICA 2025: Comprehensive Laboratory Diagnostic Solution
Case source: Dachuan District People's Hospital of Dazhou City.
01/ Backgrouno
Recently, a patient developed symptoms such as cough, fever and stethalgia, and immediately went to the Fever Clinic. The CT scan examination result of the patient showed that his lung inflammation was not obvious, and he was admitted to the isolation ward of the Infectious Diseases Department. On the next morning, the patient's condition worsened, with severe respiratory failure, accompanied by high fever and purple lips. Arterial blood gas analysis showed that the patient's oxygen partial pressure was only 43mmHg. The result of CT scan examination taken again showed that the lung lesions of the patient increased obviously, and both of his lungs were almost "occupied" in one day, and his condition progressed very rapidly.
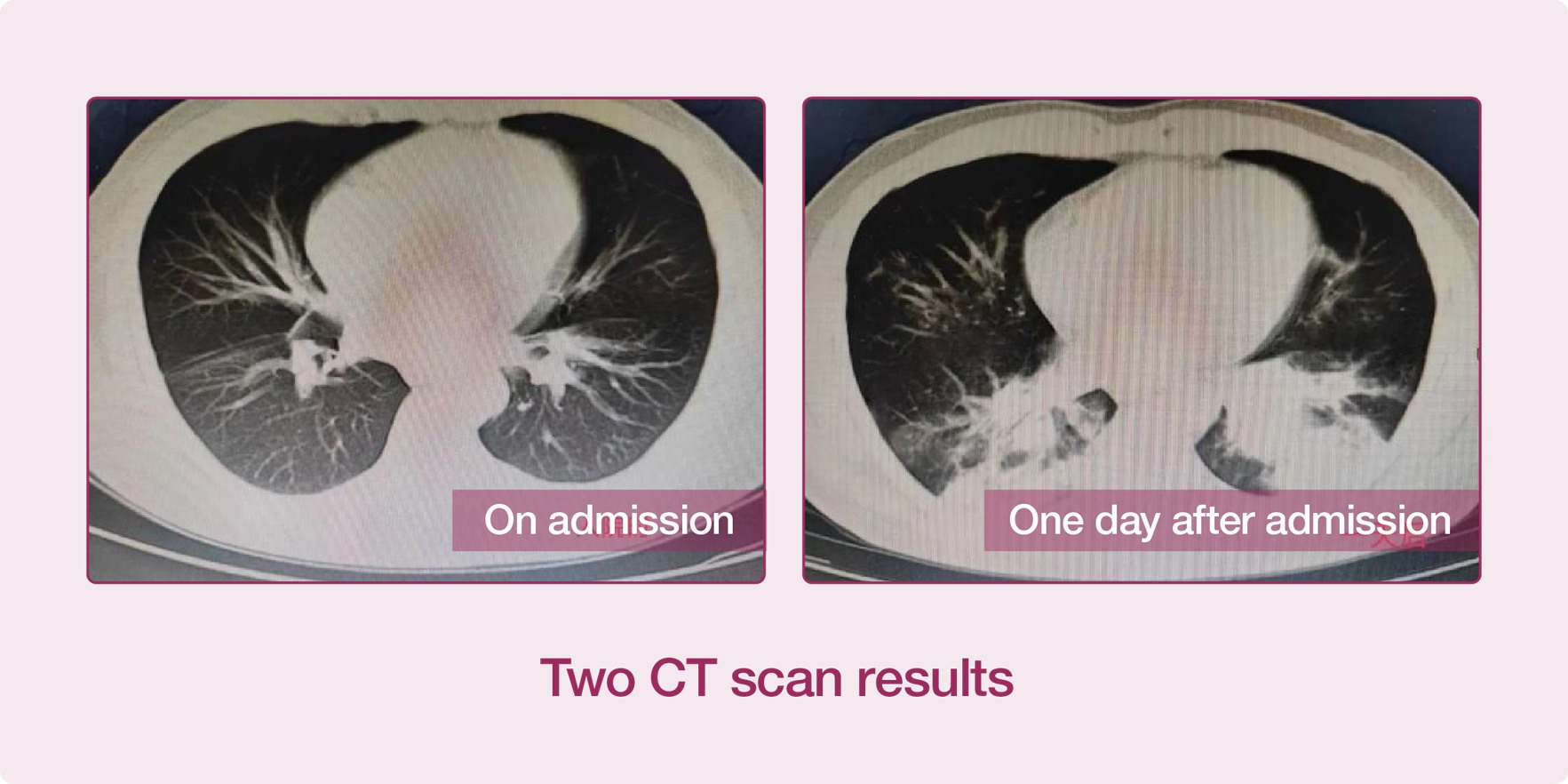
After communicating with the patient's family, the patient was immediately transferred to the ICU, and the Respiratory and Critical Care Medicine Department, the Laboratory and the Pharmacy Department were contacted for a joint consultation.
02/ Case Analysis
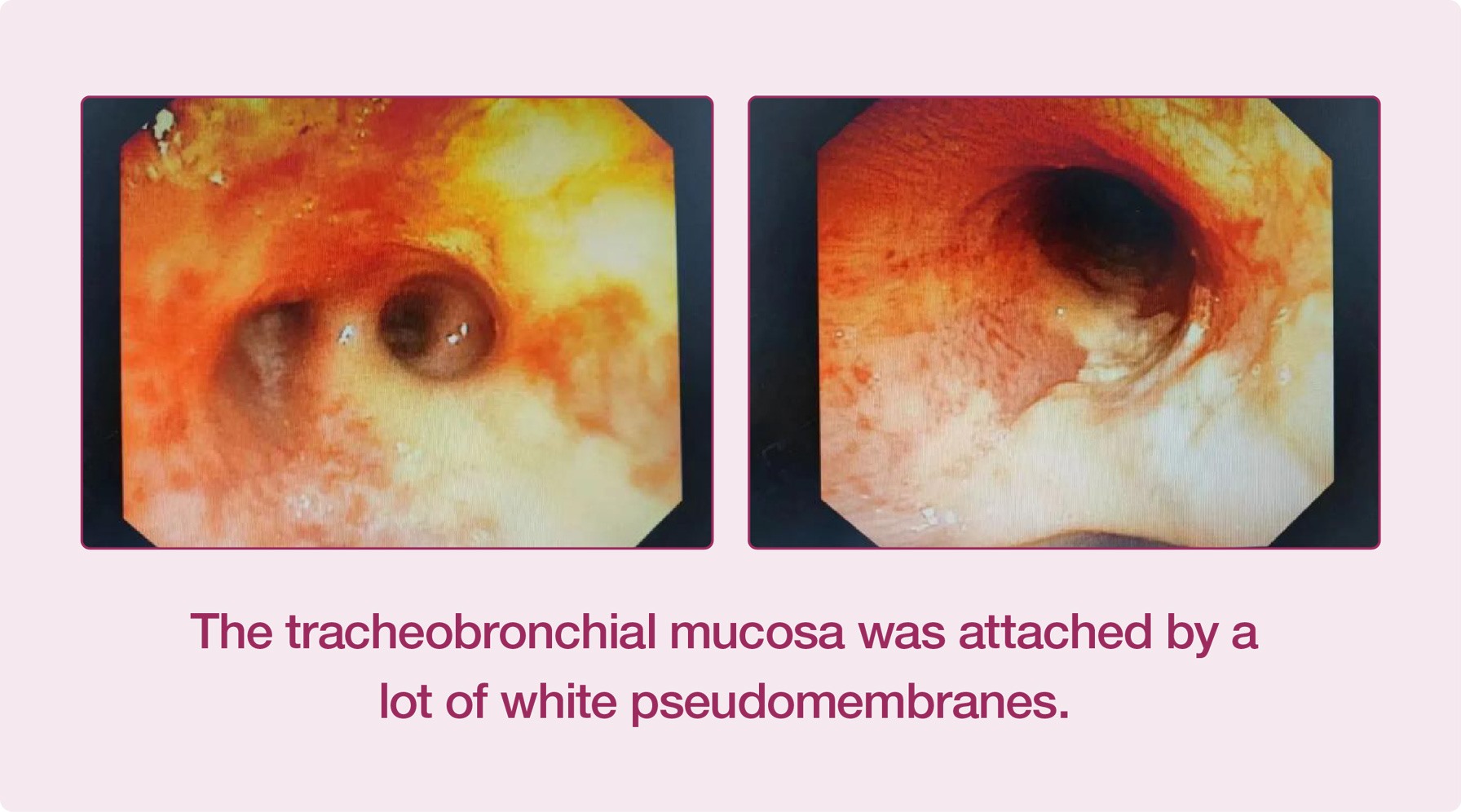
The discussions among the experts from the Respiratory and Critical Care Medicine Department, the Critical Care Medicine Department and the Infectious Diseases Department concluded that the patient had serious lung infection and airway obstruction and should take bronchoscopy urgently. The patient's bronchi were blocked by a lot of purulent sputum. After several times of sputum aspiration treatment, the patient's bronchi were unobstructed and his oxygen saturation increased. The tracheobronchial mucosa of the patient was attached by a lot of white pseudomembranes, and the lesions involved trachea and bronchus, which was extremely dangerous.
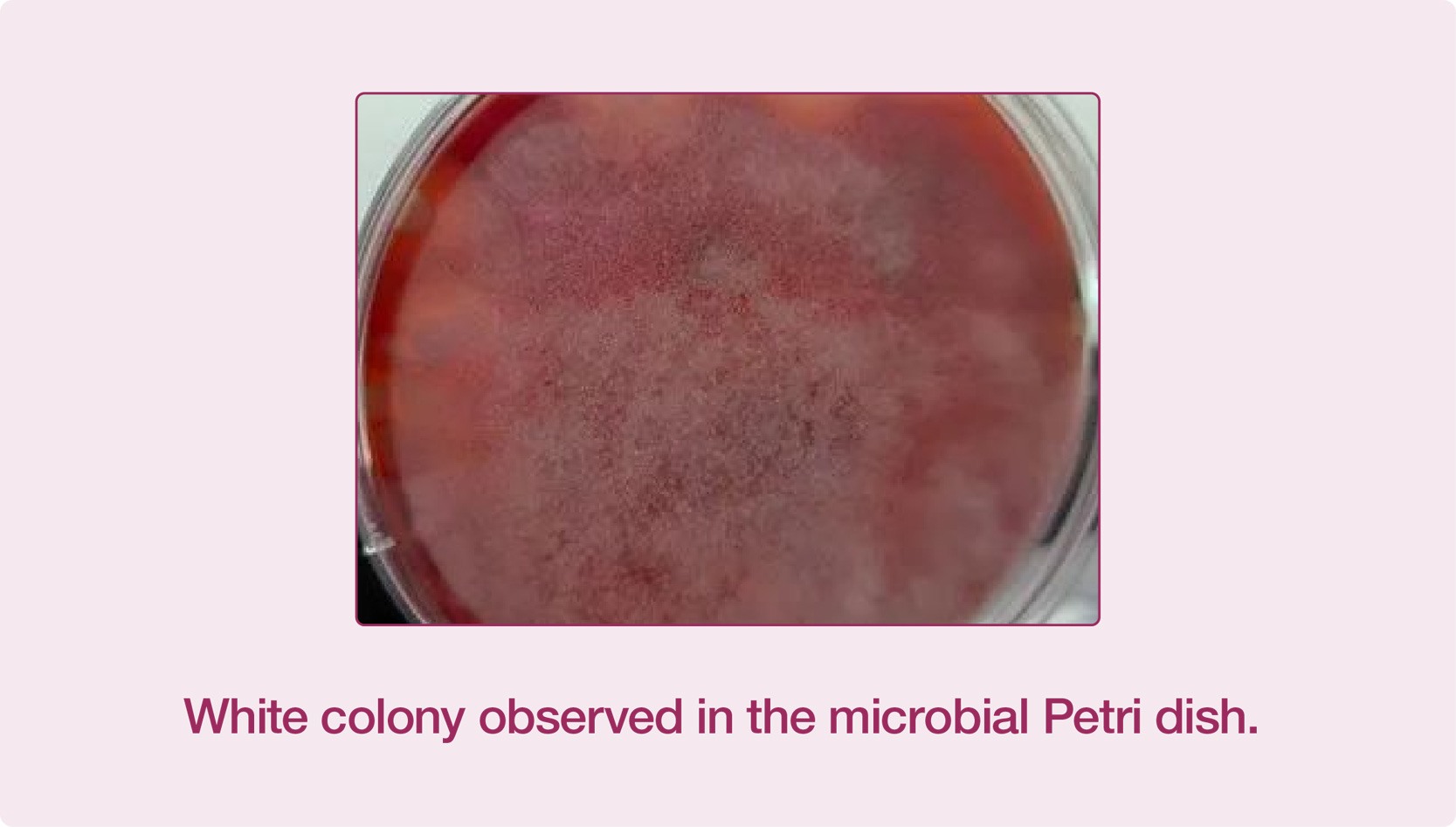
What caused the serious infection on earth? The samples were collected from the respiratory tract of the patient under bronchoscope and sent to the laboratory. With Zybio’s EXS2600 Mass Spectrometry System, the laboratory successfully detected the “real offender” — Rhizopus oryzae. Rhizopus oryzae usually leads to a disease called mucormycosis, characterized by hyphae growing in and around blood vessels. This kind of infection usually occurs in individuals with poor immune function, but it is very rare. Amphotericin B was used for the patient immediately after the clinical pharmacy consultation. The patient’s symptoms were obviously relieved, and his body temperature gradually decreased.
"Pulmonary mucormycosis is relatively rare in China, and this is also the first confirmed case in our hospital. It is difficult to diagnose this disease because it shows no specificity in clinical manifestations and imaging manifestations. The timely diagnosis of the disease this time could not be done without the cooperation of the six departments of our hospital, the application of four sets of special high-tech equipment, and the profound professional knowledge of the specialists of the six departments. Moreover, any of them was indispensable! "
"After the pathogen was cultivated, it took a few minutes for the mass spectrometer to accurately identify it and confirmed that it as Rhizopus oryzae. Compared with other routine microbe identification methods, the bacterium strain was confirmed more accurately, thus providing a strong basis for our expectant treatment and gained valuable time for rescuing the patient. This case shows the great advantages of mass spectrometry in the accurate identification of pathogenic bacteria!” The medical staff in the Intensive Care Department were deeply impressed by this aspect.

03/ Mucormycosis
Mucormycosis, previously called zygomycosis, is a disease caused by a fungus belonging to Mucorales. It is transmitted by the spores of mucor, and the most common infection route is inhaling contaminated air or taking contaminated food or via contaminated open wounds [1]. Common pathogenesis of mucormycosis include Mucor, Rhizopus, Cladosporium and Cunninghamella [2]. Mucormycosis is very rare, among which Rhizopus is the most common pathogen causing human mucormycosis, and most fatal infections are caused by Rhizopus oryzae [3].
The physical signs and symptoms of mucormycosis depend on the site of infection [4]. The infection usually starts from the mouth or nose and then enters the central nervous system through the eyes [5]. The pathogen may cause thrombosis after entering blood vessels, resulting in necrosis of surrounding tissues due to ischemia. If it infects the brain and face, it will cause unilateral headache, fever, facial ache, nasal obstruction, and other symptoms such as black mucus, nasosinusitis and conjunctival edema, etc. [5] The surface of the infected part looks normal in the initial stage of infection, and then it quickly turns red and swollen or even black due to necrosis [6]. The patient with lungs infected will suffer from dyspnea, persistent cough, hemoptysis, abdominal pain, nausea, and vomiting [7].
04/ Conclusion
Currently, there is no serological detection method for diagnosing mucormycosis [8]. Therefore, it is necessary to determine the mold in the affected tissue by biopsy and confirm it with the cultured fungi isolated from the tissue [9]. As the symptoms of pulmonary mucormycosis are similar to those of other infections, and its clinical manifestations and imaging manifestations are not specific, it is difficult for clinicians to make an accurate diagnosis of the disease rapidly. The common identification methods used in laboratory include the morphological method and the gene identification method. The former is confined by the knowledge and skills of laboratory staff, while the latter is cumbersome to operate, has higher cost, long TAT and is not suitable for routine identification.
With the continuous improvement and development of mass spectrometry, MALDI-TOF MS has played an increasingly important role in the rapid identification of fungi, especially mold, in clinical practices, and has become an accurate, rapid and economical detection method to identify mucormycosis. It only takes less than 5 min to complete the identification process. With Zybio’s 2 min mold pretreatment toolkit, the testing steps are simplified and the techniques of inactivating bacterial cell, breaking cell wall breaking and extracting protein have been improved, and more abundant protein fingerprint information can be obtained to match the database of over 350 kinds of molds, making the identification of molds more accurate and timelier.
References
[1] Reid Gail,Lynch Joseph P,Fishbein Michael C et al. Mucormycosis.[J] .Semin Respir Crit Care Med, 2020, 41: 99-114.
[2] Rinaldi M G,Zygomycosis.[J] .Infect Dis Clin North Am, 1989, 3: 19-41.
[3] Thornton Christopher R,Detection of the 'Big Five' mold killers of humans: Aspergillus, Fusarium, Lomentospora, Scedosporium and Mucormycetes.[J] .Adv Appl Microbiol, 2020, 110: 1-61.
[4] Symptoms of Mucormycosis". www.cdc.gov. January 14, 2021. Retrieved May 25, 2021.
[5] Grossman M E, Fox L P, Kovarik C, et al. Subcutaneous and deep mycoses[M]//Cutaneous manifestations of infection in the immunocompromised host. Springer, New York, NY, 2012: 1-63.
[6] Medline Plus Medical Encyclopedia: Mucormycosis". Retrieved May 19, 2008.
[7] Spellberg Brad,Edwards John,Ibrahim Ashraf,Novel perspectives on mucormycosis: pathophysiology, presentation, and management.[J] .Clin Microbiol Rev, 2005, 18: 556-69.
[8] McDonald PJ. "Mucormycosis (Zygomycosis) Workup: Approach Considerations, Laboratory Tests, Radiologic Studies". emedicine.medscape.com. Retrieved May 25, 2021.
[9]"Mucormycosis". NORD (National Organization for Rare Disorders). Archived from the original on May 26, 2021. Retrieved May 25, 2021.